Menstrual cycle: phases, hormones, average length

Reviewed by Steve Silvestro, MD, Ro,
Written by Ellyn Vohnoutka, BSN, RN
last updated: Sep 03, 2021
5 min read
Here's what we'll cover
Keeping track of your menstrual cycle can have a number of health benefits. It can help you get to know your body better and uncover health problems before they become severe.
It's also never been easier with so many period-tracking calendars and apps available.
However, to know whether you have a problem, you first need to understand how the menstrual cycle works and the common characteristics. So, here’s what you should know about the phases, hormones, and average length of your menstrual cycle.
What is the menstrual cycle?
Starting around the age of 12 years old, on average, the inner lining of the uterus begins to grow thicker each month in response to changing hormone levels in the body. This prepares the inner layer, called the endometrium, to receive a fertilized egg for pregnancy. If you don’t get pregnant that month, your body will shed the thickened lining from your body during your menstrual period (Lacroix, 2021).
The start of your menstrual cycle is affected by a complex interaction between (Lacroix, 2021):
Thyroid hormones
Adrenal hormones
Pancreatic hormones
Body fat percentages
Sex hormones
Insulin levels
Menstruation typically occurs every 21–45 days, with an average of approximately 28 days for each cycle. On average, your period will last between three to seven days. If your period lasts longer than 10 days, that’s considered “abnormal” and is a good reason to see your healthcare provider (Lacroix, 2021).
It's common for your cycles to be irregular in the first two or three years after you get your first period. Eventually, the hormone interactions in your body will balance out, and your cycles will become more regular (Lacroix, 2021).
You should continue to have regular menstrual bleeding, except when pregnant or breastfeeding, until you reach menopause, which happens when estrogen levels drop. The average age when this typically happens is between the ages of 51 and 52, though a minimal number of women (about 5%) may experience this as early as age 40–45 (Peacock, 2021).
What are the menstrual cycle phases?
The menstrual cycle is the hormonal rhythm a woman's body goes through to prepare for pregnancy each month. It includes natural changes in hormone production and the structures of the uterus and ovaries. This cycle is divided into multiple phases (Thiyagarajan, 2020).
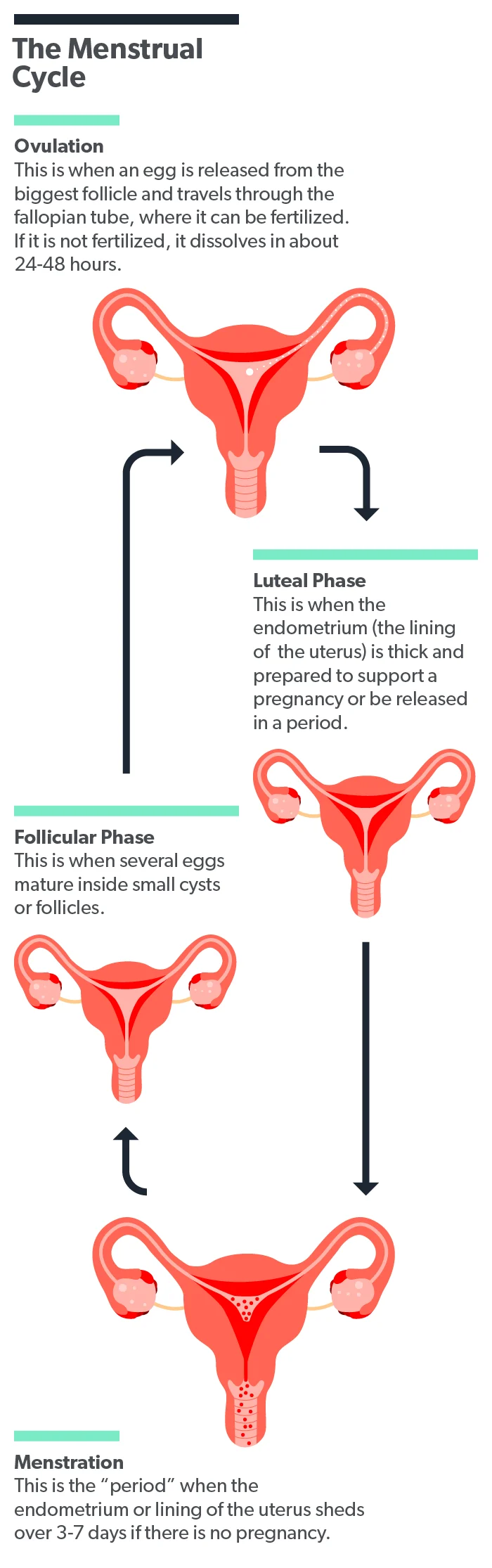
The proliferative or follicular phase
The first day that your period starts is considered day 0 of your menstrual cycle. The first phase of the menstrual cycle, called the proliferative or follicular phase, occurs from day 0 to approximately day 14. This is based on an average duration of 28 days, so the exact timing may be slightly different if your cycle is shorter or longer than 28 days. The length of this follicular phase can vary slightly and is the reason your menstrual cycle length may vary (Thiyagarajan, 2020).
The purpose of the proliferative phase is to thicken the endometrial layer of the uterus and get your uterus ready for a possible pregnancy. The primary hormone in this phase of the menstrual cycle is estrogen (Thiyagarajan, 2020).
During this phase, your body seeks to create an environment that’s friendly to possible incoming sperm. Estrogen causes channels to form within the mucus of your cervix to allow sperm to enter. At the same time, a follicle in your ovary that contains an unfertilized egg starts to mature (Thiyagarajan, 2020).
Ovulation
The release of this unfertilized, mature egg, called ovulation, always occurs 14 days before your next period begins. This means it will happen on day 14 in an average 28-day cycle (Thiyagarajan, 2020).
Your estrogen levels are highest at the end of the proliferative phase. This causes follicle-stimulating hormone (FSH) and luteinizing hormone to increase as well. These high levels of hormones cause a mature follicle in the ovary to rupture and release an egg that begins to travel towards the uterus (Thiyagarajan, 2020).
Your levels of estrogen begin to fall after ovulation is complete (Thiyagarajan, 2020).
The secretory or luteal phase
During the secretory phase, progesterone becomes the dominant hormone. This menstrual cycle phase lasts from day 14 through the last day of your cycle (day 28 for a 28-day cycle). Its purpose is to prepare your uterus for the possibility of a sperm fertilizing your egg (Thiyagarajan, 2020).
Your endometrium increases its blood supply and creates more mucus in preparation for fertilization. It also develops more complex glands, stores energy, and creates more surface area. Your body temperature increases slightly in response to this additional progesterone (Thiyagarajan, 2020).
One of two things happens at the end of this phase. If you become pregnant, the fertilized egg will implant into your uterus, and your hormones will stay elevated. If your egg does not get fertilized, your estrogen and progesterone levels drop, and your endometrium will start to break down. It will leave the body during your next period (Thiyagarajan, 2020).
What does a normal menstrual cycle look like?
When your hormone levels decrease, your body can’t maintain the thickened endometrium, and it starts to break down. This is called your period or menses (Thiyagarajan, 2020).
The length of your period can vary. The usual duration is three to five days but flows as short as one day and as long as eight are considered normal. Many factors can affect the amount of flow that you experience during your menstrual period. These include (Thiyagarajan, 2020):
Medications you take
Your hormone levels
The thickness of your endometrium
Blood disorders
Clotting disorders
Use of hormonal contraception
Premenstrual syndrome
Premenstrual syndrome (PMS) is a normal part of the menstrual cycle for many women. It’s a combination of symptoms that many women get about a week or two before their period. Studies have estimated that about 80–90% of women experience at least one symptom of PMS. They usually end a few days after your period begins (Gudipally, 2021).
Common symptoms of PMS include (Gudipally, 2021):
Changes in appetite
Weight gain or bloating
Abdominal pain
Low back pain
Breast swelling and tenderness
Nausea
Constipation
Anxiety
Irritability or anger
Fatigue
Restlessness
About 2.5–3% of women experience symptoms of PMS that are severe enough to affect their daily activities. This is known as premenstrual dysphoric disorder (PMDD). If you have symptoms of PMS or PMDD that are interfering with your life, you should see a healthcare provider (Gudipally, 2021).
What can cause an irregular menstrual cycle?
There are many reasons that your menstrual cycle could become irregular. Regular menstruation is dependent on the proper functioning of several structures and processes in the body. Changes in one of these can make your menstrual cycle irregular. These include (Lacroix, 2021):
The hypothalamus and pituitary glands in the brain
The ovaries, fallopian tubes, uterus, and vagina
Getting adequate nutrition
The absence of chronic illness
It is normal to have inconsistencies in your cycles when you first start menstruating, during and right after pregnancy, and approaching menopause. If your menstrual cycle is longer than 35 days, your period lasts 10 days or longer, or you have fewer than four periods a year, you should see a healthcare provider about irregular periods (Riaz, 2021).
All of the following could potentially cause changes to a previously regular menstrual cycle. This could mean your period is lighter or heavier than usual, or there is more or less time between your periods (Riaz, 2021; Lord, 2021).
Thyroid disease
Polycystic ovary syndrome (PCOS)
Pelvic inflammatory disease (PID)
Uncontrolled diabetes
Using birth control pills (oral contraceptives)
Some medicines such as antiepileptics or antipsychotics
Pregnancy
Breastfeeding/lactation
Perimenopause
Endometrial ablation
Sudden weight loss
COVID vaccine and menstruation
There have been some reports of menstrual cycle changes from the COVID-19 vaccines. Some women have stated that their periods are heavier for one or two cycles after receiving the vaccine. As of now, no scientific studies confirm this. However, changes to the menstrual cycle with stress aren’t unusual, and typically your cycle goes back to normal within a few months.
You should report any unexpected changes in your menstrual cycle to your healthcare provider. Depending on your medical history, your provider may order blood work or other tests to ensure you don’t have any underlying health issues.
DISCLAIMER
If you have any medical questions or concerns, please talk to your healthcare provider. The articles on Health Guide are underpinned by peer-reviewed research and information drawn from medical societies and governmental agencies. However, they are not a substitute for professional medical advice, diagnosis, or treatment.
Gudipally, P. R. & Sharma, G. K. (2021). Premenstrual syndrome. [Updated Jul 21, 2021]. In: StatPearls [Internet]. Retrieved on Sep. 3, 2021 from https://www.ncbi.nlm.nih.gov/books/NBK560698/
Lacroix, A. E., Gondal, H., & Langaker, M.D. (2021). Physiology, menarche. [Updated Mar 27, 2021]. In: StatPearls [Internet]. Retrieved on Sep. 3, 2021 from https://www.ncbi.nlm.nih.gov/books/NBK470216/
Lord, M. & Sahni, M. (2021). Secondary amenorrhea. [Updated Jul 19, 2021]. In: StatPearls [Internet]. Retrieved on Sep. 3, 2021 from https://www.ncbi.nlm.nih.gov/books/NBK431055/
Peacock, K. & Ketvertis, K. M. (2021). Menopause. [Updated Jun 29, 2021]. In: StatPearls [Internet]. Retrieved on Sep. 3, 2021 from https://www.ncbi.nlm.nih.gov/books/NBK507826/
Riaz, Y & Parekh, U. (2021). Oligomenorrhea. [Updated Aug 9, 2021]. In: StatPearls [Internet]. Retrieved on Sep. 3, 2021 from https://www.ncbi.nlm.nih.gov/books/NBK560575/
Thiyagarajan, D. K., Basit, H., & Jeanmonod, R. (2020). Physiology, menstrual cycle. [Updated Sep 17, 2020]. In: StatPearls [Internet]. Retrieved on Sep. 3, 2021 from https://www.ncbi.nlm.nih.gov/books/NBK500020/










